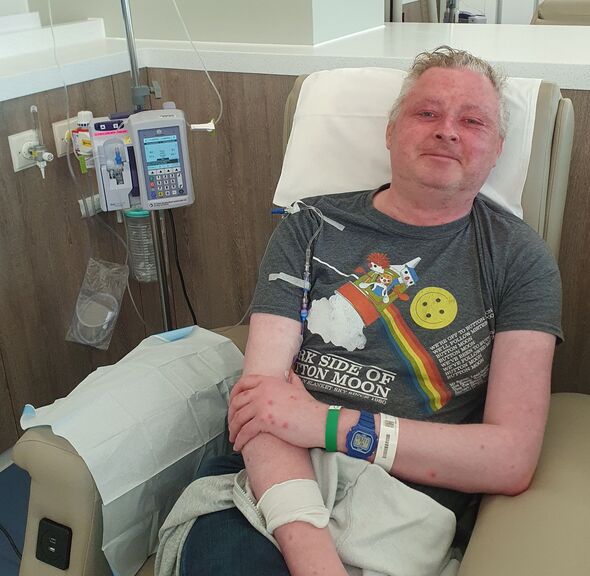
Chemotherapy is a gruelling treatment course which affects patients mentally and physically (Image: Daily Express/ Reach Plc)
When I was first diagnosed with incurable bowel cancer last summer I naively didn’t realise how it would take over my life.
From seemingly never-ending fatigue to dealing with physical and mental health challenges, it really is a constant battle.
Now, as a “chemo pro”, I’m sharing some of the things I wish I knew before I started my “cancer journey”, in the hope that they help other people.
1. Get a medical professional to fight your corner
I’m led to believe that all cancer patients are supposed to have a clinical nurse specialist that they can go to with questions and concerns about their treatment and to help them make their way through the physical and emotional minefield that is fighting the illness.

Snacks and drinks are essential to get through a chemotherapy session (Image: Daily Express/ Reach Plc)
This is great if it happens but 10 months after starting chemotherapy I still have no clue who my clinical nurse specialist is supposed to be. Instead of a contact, I have a card with a handful of names, and I believe some of those have left the team.
Thankfully I have a great relationship with my two GPs so I can turn to them for support and advice about how I’m feeling and to translate all the medical information I’m given at the cancer hospital.
Whether you rely on your GP for support or a clinical nurse specialist, or someone else on the team, there will be someone out there to help you understand what is going on.
2. You’ll need to be your own personal assistant
The amount of medical appointments you’ll attend is absolutely immense, as your medical team tries to assess whether the drugs are doing their job.
Usually, on a chemo week, I’ll have an appointment for blood tests, then observations like blood pressure and weight, before a meeting with someone in my cancer treatment team to discuss the results and to see if chemo can go ahead.
Dr Anisha discusses Bowel Cancer symptoms
The next day is taken up with around six hours in the day unit having chemotherapy. This is followed by an appointment two days later to have my chemotherapy pump removed.
That’s only five appointments but some weeks, with CT scans and other tests, having 10 medical things to get to isn’t uncommon.
My proudest day was when I managed to start with a GP appointment in Croydon, South London, then get to my cancer hospital in Sutton for three appointments, including the aforementioned blood tests, before going back to Croydon for different blood tests.
I then very importantly made sure I had time to have cake at the hospital’s Costa Coffee.
3. Some hair loss will happen
My hairdresser used to say my hair wasn’t fifty shades, but two shades of grey with quite a bit of brown.
It used to be thick and luscious but chemotherapy has zapped it of life and now it feels thin, curly, and wiry, like stroking a sheep.

This drug gradually flows into my body over 46 hours (Image: Daily Express/ Reach Plc)
This comes after the lead cancer doctor told me the treatment plan I’m on wouldn’t cause hair loss.
It obviously hasn’t caused all of my hair to fall out but I wasn’t prepared for odd patches of hair on my body to just drop out and then to grow back very slowly as stubbly bits, and for me to now look a lot older and greyer than I think I am.
4. You’ll have to work to keep your identity
With so many medical appointments to fit in and so many side effects and symptoms to deal with, it can be difficult to see yourself as anything other than someone who has cancer.
I realise that cancer is now a big part of who I am, especially as it is the thing that will probably kill me. But I’m still working hard to ensure it isn’t the thing that defines me.
I treat it like a top secret job so I don’t really talk to friends about how things are going with treatment and instead talk about other much more interesting things in life.
It’s important for me to still be seen as a friend they can have fun with, instead of someone who is going to go on about being ill all the time.
Obviously, it’s vital to have friends there for support when needed, but sometimes the best support is an hour or two when I’m not worrying about whether my magnesium levels will be too low.
Each chemotherapy sessions usually takes me at least six hours so I put my feet up (Image: Daily Express/ Reach Plc)
5. Chemotherapy nausea is a bit like a bad hangover
I gave up drinking just before starting chemotherapy to give my liver the best chance of success at breaking down the toxins without having to deal with alcohol too.
But delightfully I still get to experience hangover type symptoms every time I finish chemotherapy and try to work out whether I’m feeling okay enough to have some dinner.
Usually, I manage to have a Scotch egg or a sandwich but one time I was feeling okay so I treated myself by ordering a pizza. This would have been fantastic if my hangover-style nausea hadn’t kicked in by the time the delivery arrived and I felt too ill to try a slice so I had to put it all in the fridge.
Sleep and the anti-nausea medicines you get given at your hospital are the best way to reduce the feelings of post-chemo sickness.
6. Everything takes ages to heal
This should have been obvious to me from the start as the chemotherapy works by destroying fast-growing cells, with the aim of decreasing the rate that the cancerous cells grow.
But for some reason, it always comes as a surprise when cuts on my feet and hands (thanks to the cancer treatment for drying out my skin) take weeks rather than days to heal.
My ‘favourite’ healing process was after I fell backwards in my bedroom a few days before Christmas. I’d been trying to stay warm by putting a pair of trousers on over some other trousers when I lost my balance and smashed my back and arm against my bed.
It took several minutes before I could get up and then an agonising few weeks, including two GP appointments and two with a physiotherapist, before I was healed.
This would have been healed in a matter of days if I didn’t have cancer and wasn’t going through chemotherapy.
So the main message here is to accept your limitations while having chemotherapy. You won’t be able to do everything you did before and you certainly shouldn’t try and wear trousers over trousers just to save a few pennies on your heating bill.











